Paper-based medical records slow down care, increase errors, and waste staff time. At Scan N More, we’ve seen firsthand how medical records digitization transforms healthcare operations.
Digital conversion eliminates filing delays, reduces lost documents, and gives clinicians instant access to patient information. The shift from paper to digital isn’t optional anymore-it’s what modern healthcare demands.
Why Medical Records Digitization Matters
Patient Safety Depends on Speed
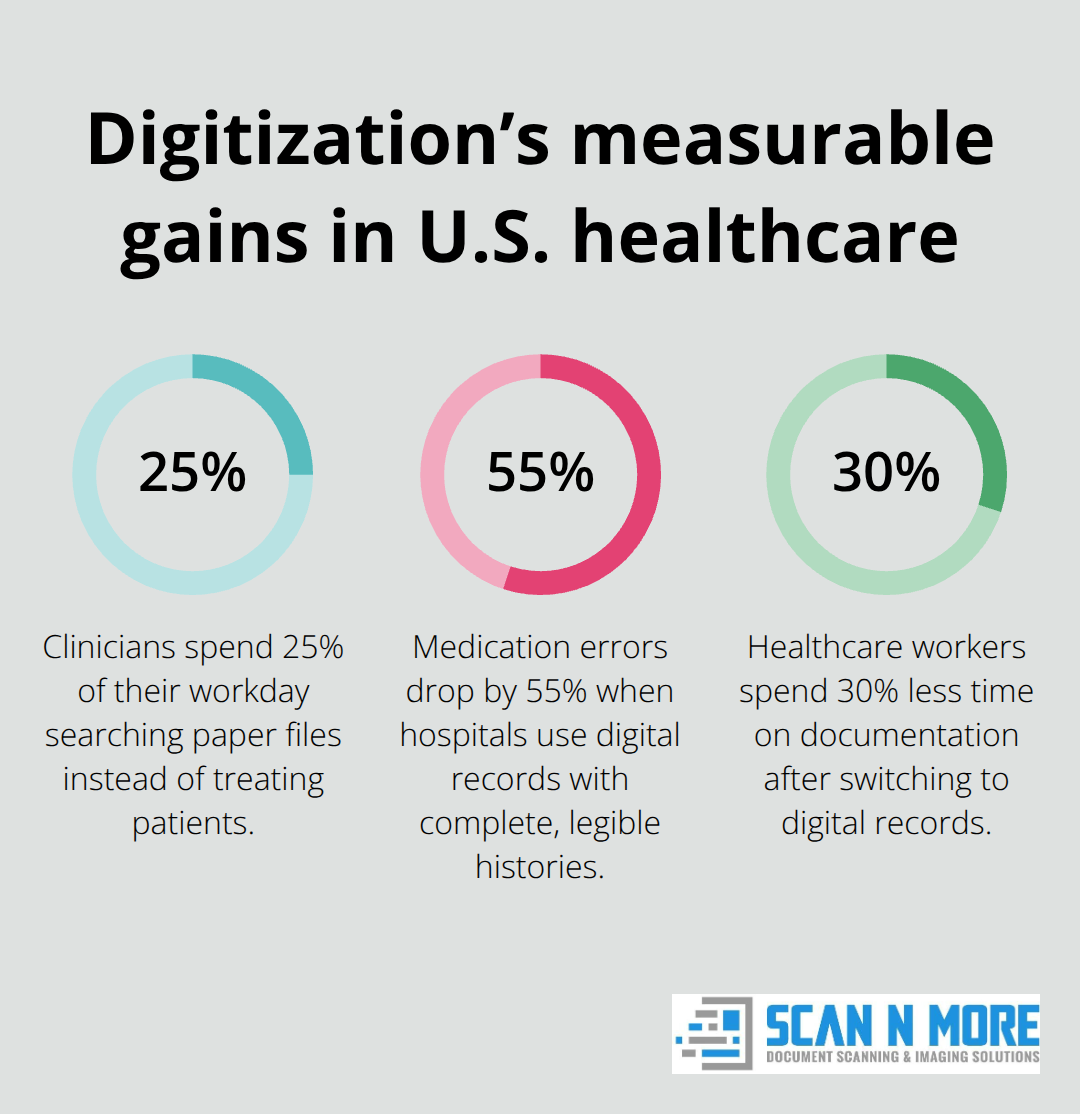
Patient safety hinges on speed and accuracy. Clinicians spend 25% of their workday searching for patient information across paper files, time that should go toward diagnosis and treatment. The American Medical Association found that physicians spend an average of two hours per day on administrative tasks tied directly to paper records management. Digitization cuts this dramatically.
When a cardiologist needs a patient’s previous EKG results during an emergency, digital records eliminate the gap between knowing and acting. Paper creates delays that compound into missed diagnoses and medication errors. Digital systems provide clinicians the information they need the moment they need it, transforming how fast teams respond to critical situations.
Financial Impact Hits Immediately
The cost argument for digitization stands on solid ground. Healthcare facilities face significant costs for storing and managing paper records. A 500-bed hospital with 50,000 active patient files spends substantial resources on storage, retrieval, and staff time.
Digitization requires upfront investment, but the payoff appears within 18 to 24 months through reduced storage costs, fewer lost documents, and staff time redirected toward patient care instead of filing. The American Hospital Association reports that practices switching to digital records recover 30% of administrative costs within two years. A single medication error costs healthcare systems an average of $5,000 to $10,000 in additional treatment and liability exposure. Digital systems with built-in verification reduce these incidents significantly.
Access Transforms Care Coordination
Specialists coordinating care across multiple facilities operate in the dark with paper records. Cardiologists cannot see what the primary care physician observed. Surgeons perform procedures without complete medication histories. Digital records shared across authorized providers eliminate these dangerous gaps.
When a patient moves between departments or facilities, their complete medical history follows instantly. This accessibility transforms how teams approach complex cases and prevents duplicate tests that waste money and patient time. Authorized providers gain the full picture they need to make informed decisions quickly, improving outcomes across the entire care continuum.
The foundation for better outcomes rests on how well your organization handles the actual conversion process itself.
How to Execute Medical Records Digitization Without Disrupting Care
Select the Right Scanning Partner
Selecting a scanning partner matters more than most healthcare leaders realize. The wrong choice creates bottlenecks, security gaps, and incomplete conversions that leave your organization worse off than before. What separates successful digitization from failed projects is choosing a partner with healthcare-specific expertise, not just general document scanning capabilities.
Your vendor needs to understand HIPAA requirements built into their workflow, not as an afterthought. They should handle medical imaging formats, manage chain-of-custody documentation, and provide audit trails that regulators actually expect. A 200-bed hospital digitizing 500,000 patient records needs a partner equipped for on-site and off-site scanning operations, depending on your security comfort level.

When evaluating partners, ask about their HIPAA compliance certifications, experience with records of your volume, timeline capacity, and whether they conduct hard drive destruction for temporary data storage. Healthcare organizations that work with specialized vendors experience fewer compliance issues than those using general scanning companies lacking healthcare infrastructure.
Plan Your Transition in Phases
The transition itself requires careful planning around your patient volumes. Most healthcare facilities cannot shut down operations for digitization, so phased approaches work better. Starting with inactive records from the past three to five years lets your team test workflows without affecting current patient care.
Active records transition during lower-volume periods or in departmental waves. A cardiology practice might digitize their records first, allowing staff to adapt to digital workflows before oncology and primary care follow. This staged method typically takes three to six months for mid-sized practices and up to eighteen months for large hospital systems.
Maintain parallel systems during transition because paper and digital coexist until conversion completes. Staff resistance drops when clinicians see speed improvements immediately. Practices that implement phased transitions experience faster staff adoption compared to big-bang conversions.
Maintain Compliance Throughout the Process
Your compliance framework cannot wait until digitization ends. HIPAA requirements apply throughout the process, not after. Your scanning vendor must maintain secure transport, encrypt data in transit and at rest, and limit access to authorized personnel only.
Document everything. Audit logs showing who accessed what records and when become your legal protection. Healthcare organizations face fines averaging $100,000 to $50,000,000 per HIPAA violation depending on severity and negligence level, according to the Department of Health and Human Services enforcement actions. A single breach notification costs money in addition to regulatory penalties.
Handle Legacy Records With Quality Standards
Legacy records present their own challenge. Medical records from decades past may exist in various conditions, formats, and organizational systems. Some files are water-damaged, faded, or incomplete. Your digitization vendor should have quality control protocols that flag illegible documents before they enter your digital system.
Establish standards upfront for how you handle problem documents. Will you request original records from patients? Will you note legibility issues in the digital file? These decisions prevent downstream problems when clinicians encounter poor-quality scans during patient care.
Calculate Your Investment Timeline
The investment timeline deserves realistic expectations. Upfront costs include equipment, labor, and vendor fees. A 500-bed hospital typically invests $150,000 to $300,000 for comprehensive digitization including infrastructure upgrades. Smaller practices spend $20,000 to $50,000 depending on record volume.
The payoff arrives through reduced physical storage costs, recovered staff time, fewer lost documents, and prevented medical errors. Most organizations recoup their investment within two years through operational efficiencies alone. Once your systems go live, the real measure of success appears in how your staff and patients experience the new digital environment.
Real-World Impact of Medical Records Digitization
Medication Errors Drop Sharply
Medical errors fall measurably once paper records vanish from clinical workflows. A study by the National Coordinator for Health Information Technology found that medication errors reduced by 55% in hospital settings because clinicians access complete, legible medication histories instantly instead of deciphering handwritten notes. When a nurse administers medication, they see every allergy, interaction, and previous adverse reaction on screen within seconds. Paper records sit in filing cabinets while patients wait. Digital systems eliminate that gap entirely.
The financial impact compounds quickly. Medicare data shows that hospitals preventing just five medication errors per month recover their digitization investment faster than projected. A single medication error costs healthcare systems an average of $5,000 to $10,000 in additional treatment and liability exposure, making error prevention a direct financial win.
Diagnostic Accuracy Improves Immediately
Diagnostic accuracy improves because radiologists and specialists access prior imaging and lab results without requesting them from other departments. A cardiologist reviewing a patient’s history finds previous stress tests, EKGs, and echocardiograms already loaded in the system, enabling faster and more informed clinical decisions. Specialists no longer wait for records to arrive from other facilities or departments, which means they make decisions based on complete information rather than incomplete data.
Staff Efficiency Gains Appear Within Weeks
Staff efficiency gains appear within the first month of going live, not years later. Clinicians stop wasting time on administrative work and focus on patients. A systematic review of the literature examining the impact of electronic health records on documentation time found that healthcare workers spend 30% less time on documentation tasks after switching to digital records because templates, auto-populated fields, and structured data entry replace manual searching and typing.
Front desk staff no longer spend hours locating misfiled records or calling other departments to track down patient information. Patient satisfaction scores climb because visit wait times shrink when records load instantly instead of requiring staff to retrieve physical files from storage. Appointment scheduling becomes faster because staff access complete patient histories without delays. Insurance verification happens in real time instead of requiring follow-up phone calls.

Patient Experience Transforms
Patient satisfaction increases by 20-30% according to healthcare IT benchmarking data, and staff overtime hours drop significantly because workflows move faster. Digitization also enables better inventory management of physical storage space, freeing real estate previously dedicated to filing cabinets and records rooms that can now serve patients or support operations more effectively. Patients experience shorter wait times, faster appointment scheduling, and more attentive clinicians who spend their time on care rather than paperwork. Organizations that implement digital systems see increased productivity, lower storage expenses, and faster information retrieval that directly enhance the patient experience.
Final Thoughts
Medical records digitization delivers measurable returns that extend far beyond the initial investment. Healthcare organizations gain faster access to patient information, reduce medication errors by 55%, and recover administrative costs within two years. Clinicians reclaim hours previously lost to filing and searching, redirecting that time toward actual patient care.
The path forward requires selecting a partner who understands healthcare compliance from the ground up. General document scanning companies lack the infrastructure for HIPAA requirements, medical imaging formats, and audit trails that regulators expect. Your vendor needs healthcare-specific expertise built into their workflow, not added as an afterthought, and should handle on-site and off-site operations with transparent pricing.
Phased transitions work better than attempting full conversion overnight, and Scan N More specializes in helping healthcare organizations transition smoothly with professional document scanning services that maintain HIPAA compliance throughout the process. Contact a digitization partner experienced in healthcare, establish your compliance framework upfront, and plan your phased transition to see benefits appear within weeks.
